— Verve Patient
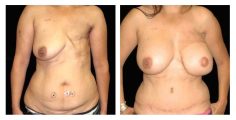
DIEP flap
Sometimes a mastectomy or radiation therapy will leave insufficient tissue on the chest will to cover or support a breast implant. In these cases, breast reconstruction usually requires a flap technique, also known as autologous (your own tissue) reconstruction.
What Is a DIEP Flap?
DIEP stands for Deep Inferior Epigastric Perforator flap; this name comes from the vessels in the abdomen which are needed in order to perform this “free flap” type of reconstruction. The blood vessels from the abdominal tissue are reattached to the blood vessels in the chest so the flap can develop its own blood supply and thrive. The abdominal tissue is then shaped into a natural looking breast.
Image Transcript:
Who Is a Good Candidate?
- You plan to have a mastectomy and do not want breast implants.
- Has history of radiation therapy.
- Has failed implant reconstruction and/or other autologous reconstruction.
- Has excess skin and tissue on the lower abdomen.
- A special CT scan will be needed to evaluate the diameter of the blood vessels in your chest and in your abdomen. These vessels need to be large enough to sew together under a microscope, ideally 2mm or larger. Dr. Gupta will order this scan for evaluation.
- You should be at or close to your ideal weight, with a BMI less than 35.
- The best candidates are non-smokers. Smoking increases the chance of complications including impairment in wound healing.
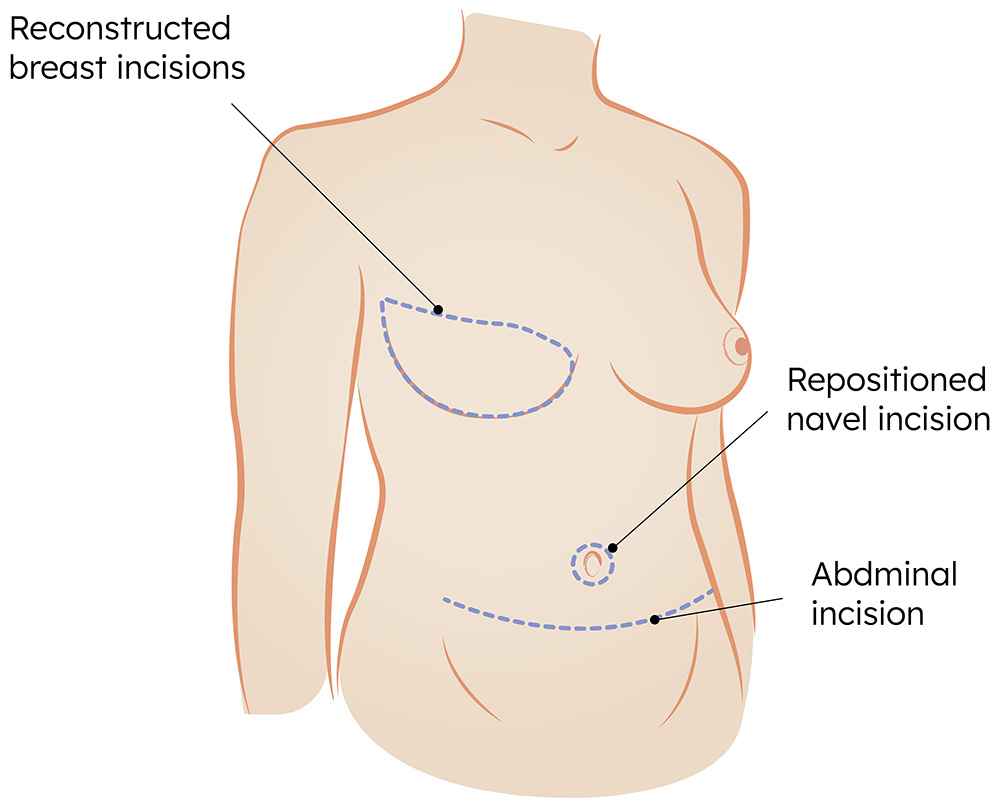
The Incisions
- A horizontal incision is made in the low belly near the pubic area (or prior C-section scar if applicable). The length of the incision depends on the amount of skin that needs to be removed. A new opening will be made for the belly button. You will have a circular scar along the belly button.
- You will also have an elliptical incision on the breast where the new tissue will be placed.
The Procedures
- You will see Dr. Gupta prior to surgery, he will draw his surgical plan on your abdomen and breast.
- The duration of surgery often rages from 6-9 hours, depending on the complexity of the case.
- During surgery Dr. Gupta will first evaluate the blood vessels in the chest. He will explore and dissect these vessels ensuring they are patent enough and have a large enough diameter to sew the abdominal vessels to. After the chest vessels have been evaluated and prepared Dr. Gupta will begin to raise the lower abdomen flap.
- An incision will go from hip to hip in along the lower abdomen. Fat and skin will be raised leaving the rectus muscle attached. The DIEP vessels will be detected and carefully dissected through the muscle; these vessels are evaluated to ensure they are a large enough caliber to sew to the chest vessels.
- When the vessel has been evaluated and completely dissected, the flap is completely detached from the body.
- The abdominal incision is closed quickly in multiple layers to provide a strong and secure closure. Time is of the essence as the flap is not currently receiving any oxygenated blood. (remember its completely detached from the body)
- As soon as the abdomen is closed, the free flap is placed into the chest.
- Using a microscope, the vessels are sewn together very carefully, the anastomosis is checked for patency. The flap will be evaluated to ensure that blood is flowing in and out of this new connection.
- These newly connected vessels are the only blood supply to the flap. Over the next few months new blood vessels will develop to help supply nutrients to the flap.
- Once the flap has been established as viable the breast incisions will be closed. A special monitor will be placed on the flap to evaluate the blood flow to the area, this will remain in place for your entire hospital stay.
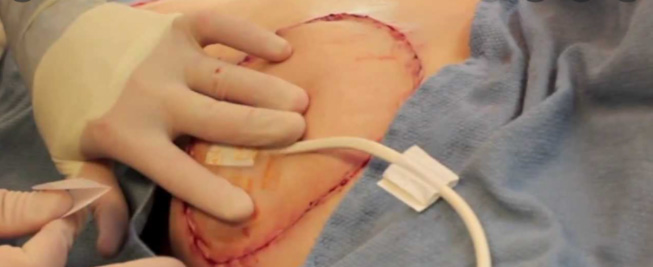
- The flap is very vulnerable in the first few days after surgery. ICU care is required to evaluate the flap every 1 hour, if there are changes in the flap such as color change (darkening) & decreased oxygenation on monitor readings, an emergent surgery may be required to re-evaluate the connection between the vessels. Dr. Gupta will be on call after your procedure and can be reached by the ICU nurses at any time in case his evaluation is needed.
- In the ICU the goals will be pain control and monitoring the flap. The abdomen will be sore, and you will need to remain in a flexed position. We will have you evaluated by a physical therapist to ensure you are ambulatory as soon as possible.
- Depending on the appearance and stats of the flap, you will remain in the ICU. Until 3 days post op. It is then safe to decrease the frequency of flap checks to every 4 hours, at this time you will be transferred to an Acute care floor in the hospital.
- You will be discharged 5 days after surgery. All of your post op medications will be sent to your pharmacy. You will go home with the surgical drains in place.
FAQs
Yes. You will stay in the hospital 5 days, typically 3 days in the ICU.. Y
Yes. The purpose of the DIEP flap is to ensure the newly transplanted tissue survives. No additional breast contouring will be performed at this time as it can compromise the success of the flap.
Yes. 1 drain in the breast and 2 drains in the abdomen. They will stay in place 1-3 weeks depending on the volume of fluid output.
Request an Appointment
Call (760) 436-7600 or fill out the form to schedule an appointment to discuss your needs in detail